In August of 2016, at the end of a long, dark period in Ahmed Haider’s life, his niece from Bangladesh visited him in Toronto. Haider and his wife, Hosne Afroz, took their guest on a grand tour of southern Ontario: Niagara Falls, the CN Tower, the Woodbine Racetrack. They also drove past the Lowe’s store where Haider had an evening job in the greenhouse. His oldest of two sons, aged six, pointed excitedly from the backseat: “Look, my dad’s a gardener.”
That evening, Afroz was inconsolable. “Your son will never know you’re a doctor,” she said, weeping. “You’re losing your identity.” Haider tried to reassure her. “I have many identities,” he said. “I’m a human being. I’m a father.” But he shared her despair. He hadn’t donned a stethoscope since arriving in Canada in 2012 and wondered if he ever would again.
When Haider emigrated from Dhaka, he was 33. He’s pushing 40 now but looks younger — a long-bearded, soft-spoken man with an ingenuous smile. Afroz, whom Haider describes as “brilliant,” is also a doctor, earning her degree at one of the country’s most prestigious schools, the Sir Salimullah Medical College in Dhaka. In 2012, the couple got their Canadian immigration papers through the Express System program — commonly referred to as the “points system” — which offers expedited visas to people like them: healthy, credentialed, and not too far into their working years. The points system holds out a special promise for immigrants. Surely, any country that so heavily emphasises professional skills must also be one in which newcomers can land good jobs.
The couple and their two young sons settled near Victoria Park Station, in a community sometimes called Little Bangladesh. The area straddles two neighbourhoods of the east sub-region, Oakridge and Taylor-Massey (formerly Crescent Town), and has sizable migrant populations from India, Pakistan, and other South Asian countries. At its centre is a suite of concrete high rises built in the postwar tower-in-a-park style. There’s ample green space, in which one sees picnics and cricket matches on weekends. The towers have prayer rooms oriented toward Mecca, and there’s halal meat for sale at the local grocery stores.
Haider’s first two years in Canada were promising, at least professionally. In fall 2013, with money from home, he enrolled at the Mennonite New Life Centre in a bridge training program, which acquaints newly arrived doctors with Canadian health-care protocols. Although not a licensed physician in Canada, he began working as a counsellor at Mennonite. Thanks to a partnership with his local Bangladesh Centre and Community Services agency, he also worked one day per week in his neighbourhood.
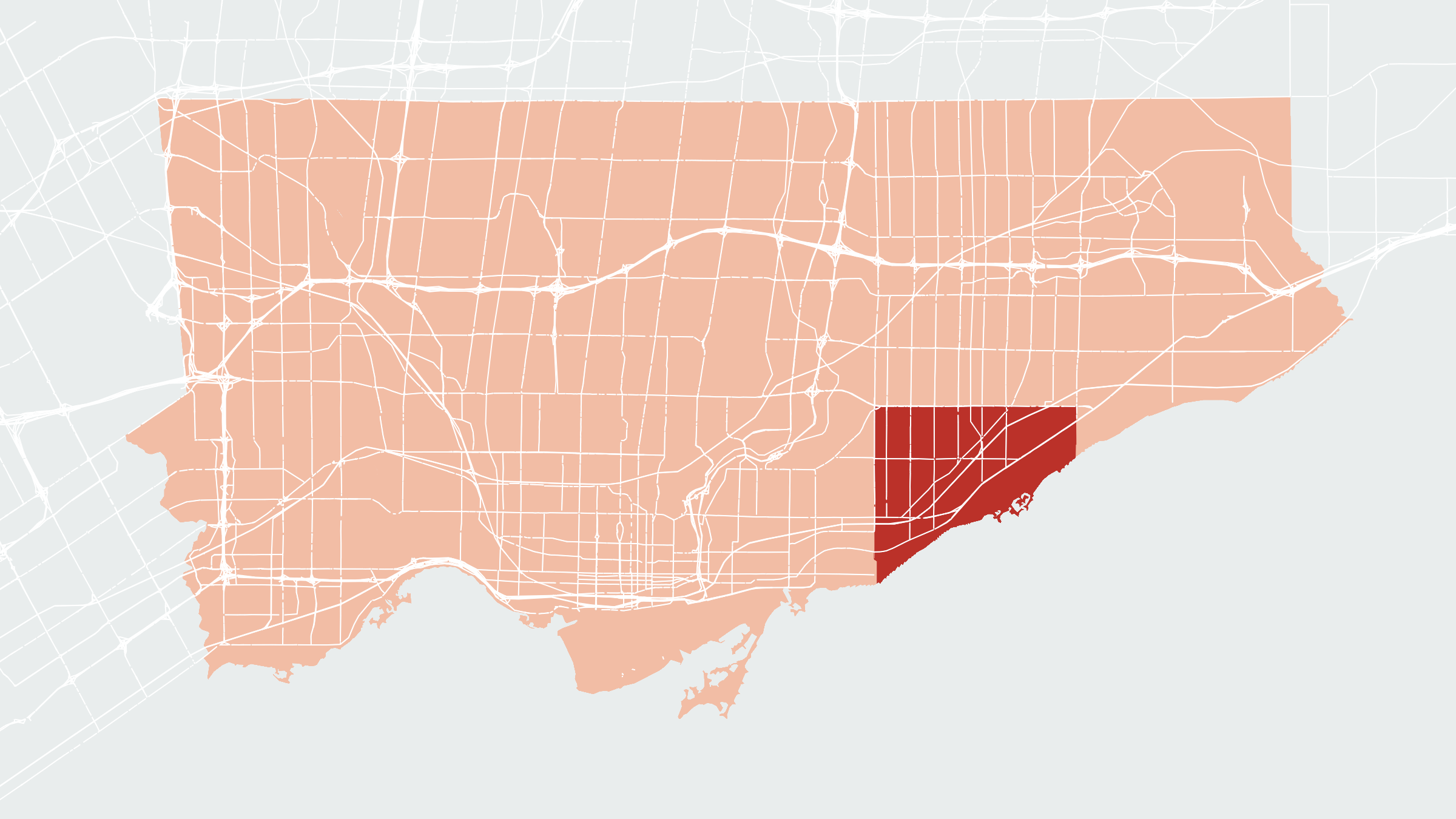
The job put him in the centre of a community reeling from a mental-health crisis. Out of the city’s 72 neighbourhoods, Taylor-Massey has the highest rate of mental-health visits per year; Oakridge isn’t far behind. Haider believes that residents’ inability to find work in their fields is a leading contributor to these ailments. The research bears him out. In a forthcoming York University study on the Bangladeshi community, numerous participants reported that “lack of job security, precarious employment, and lack of meaningful employment upon arrival were the greatest source of stress and frustration in a new immigrant’s life.”
To understand the relationship between employment and mental health, one must appreciate both the importance of work in South Asian cultures and the ways in which work impacts every other facet of a person’s life. As a counsellor, Haider witnessed these dynamics. Then he lost his job, and the problems of the community became his problems too.
Researchers who study mental health in immigrant populations often focus on two types of stress: pre-migration factors (the difficulties people encounter in their countries of origin) and post-migration factors (the challenges people face in their adopted countries, which can magnify pre-existing problems). “Everyone who comes from Bangladesh carries a certain amount of trauma with them,” says Farah Islam, a community health researcher who focuses on Bangladeshi Canadians.
Bangladesh is a small country with a huge number of people: imagine half of the US population on a land mass the size of Illinois prone to cyclones, floods, and tropical diseases. In 1971, Bangladesh separated from Pakistan after an eight-month war, during which communities were subjected to mass murder and rape. “My mother-in-law still has nightmares about that time,” says Islam. “It’s very much in the consciousness of people collectively.”
Few citizens have contact with mental-health services. The country has one psychiatrist for every 1.4 million people, and the ratio of psychologists to citizens is a starker one-to-14-million. The Pabna Mental Hospital — a dilapidated, overcrowded facility that is one of two psychiatric clinics in the country — looms large in the popular imagination, just as old Hollywood depictions of Bedlam do in Anglo-American culture. “People think, ‘that’s where insane people go to be locked up,’” says Islam. “We have a very scary idea of mental illness.” Mentally unwell people, she says, are referred to as pagol, which translates, roughly, to crazy.
In Bangladesh, Haider saw patients who struggled to articulate their inner turmoil. “Lots of people came to me with physical issues, but when I investigated, I didn’t find anything physically wrong,” he says. He remembers a woman who suffered from chronic pain but hadn’t been able to get a satisfactory diagnosis, despite consultations with multiple specialists. Unable to help her medically, Haider talked with her instead. The women eventually told him something she’d never shared with a physician: Her pain began when her son, a migrant labourer in Saudi Arabia, died in a car accident and the Saudi authorities refused to repatriate him. “I can’t even see my son’s dead body,” she said. Haider believes that her unspoken trauma contributed to her physical ailments.
In Canada, Haider discovered, getting people to talk about mental health was as difficult as it had been in Bangladesh. “Stigma manifests slightly differently in South Asian populations than it does elsewhere,” says Gursharan Virdee, a research analyst at CAMH who co-leads the Collaborative for South Asian Mental Health. “Communities are collectivist, which means stigma is a collective phenomenon. If somebody is experiencing a mental-health issue, they’ll worry not just about how it affects them but also how it impacts their family’s standing.”
This collective ethos can be a source of support: newcomers tap into familial networks, and working-age adults take care of their aging relatives. But the community approaches mental health as a familial, and therefore secretive, affair. While conducting research in the Peel Region, Virdee met a woman who worried that her schizophrenia diagnosis would undermine her sister’s marriage prospects.
Familial stigma, the fear of being labelled pagol, and a lack of experience with preventative psychiatry — these factors feed into a culture of silence. When Haider first began counselling in the Oakridge area, he distributed flyers offering mental-health services. After failing to get responses, he spoke to a settlement worker who advised him to remove the words “mental health” from the document. “She told me to use the phrase ‘supportive counselling’ instead,” he explains.
Soon, he’d built up a small but steady roster of clients, whose challenges included depression, anxiety, drug and alcohol problems, and in one case, a videogame addiction. Where possible, he referred people to psychiatric services and encouraged them to see their challenges not as personal failings but as responses to life stresses.
Haider also observed the close connections between employment and mental wellbeing. Vocational stress is tough in and of itself, but it also intensifies the many other difficulties that new immigrants face. When people fail to find jobs to match their skills, and instead accept manual labour or service work, the experience is not only demoralizing but also disruptive. It frays relationships, shortens tempers, undermines family power structures, and inhibits people’s ability to cope with the many other challenges of immigrant life.
As a counsellor, Haider noticed a common pattern: men would fail to find work and then struggle, psychologically, when their wives became breadwinners. “Suddenly, the wife’s earning, and she wants to be part of the decision-making,” he explains. “The husband believes he’s losing control.” Studies show that, in the worst-case scenarios, these tensions can culminate in domestic violence, which inevitably affects the mental health of spouses and children.
When people fail to find jobs to match their skills, it frays relationships, shortens tempers, and inhibits people’s ability to cope with the many other challenges of immigrant life.
Poverty itself is both a source of tension and a barrier to seeking help. Islam’s research shows that as financial and employment pressures mount, people tend to prioritize the immediate issues — jobs and money — over their psychological health. Sometimes men who earn low wages will compensate by pulling long hours, estranging them from their families. The situation can be devastating, but it’s also, cruelly, inevitable, given the rising cost of living. “When I came to Canada in 2012, a one-bedroom unit in my neighbourhood was $860,” says Haider. “The same unit is now more than $1,000.”
As a counsellor, Haider’s worst regrets were the people he couldn’t reach. He remembers a woman dealing with domestic abuse. “Her husband hit her with a belt on her shoulder,” he recalled. “She didn’t go to the doctor, because she feared a call to the police.” The woman wanted her husband to seek mental-health counselling but was afraid to broach the subject with him. Instead, she asked Haider if he’d visit her husband at home, perhaps claiming to be a distant relative. Haider wanted to honour this unorthodox request, but his manager explained that he was uninsured to do house calls. “I didn’t want to say no to her,” he says of the women, regretfully.
In 2015, halfway into the job at Mennonite, the executive director informed Haider that his funding had not been renewed. He would need to leave once his 11-month term ended. Haider had barely settled into his borrowed office near Oakridge — “I only had a few piles of paper there,” he says — but he was heartbroken to say goodbye to his clients.
That summer, Afroz applied for residency after residency — competing with foreign-trained doctors from around the world for a limited number of precious spots, growing increasingly worried that she was falling out of practice. Haider, in the meantime, took care of things at home. Every morning, he drove his son to classes at Finch Avenue and McCowan Road. At 3 p.m. he drove back for pick up. To pay the bills, he took evening jobs, returning to the kind of manual labour he’d done during his very first days in Canada.
His first job was at a cookie factory. “The work wasn’t hard, but it was fast,” Haider recalls. “And if you made a mistake, the assembly line would stop. Some ladies there were faster than machines. When I couldn’t keep up, they’d swear at me.” His next job — the last before he was hired at Lowe’s — was in a massive Jack Astor’s kitchen, which he hurriedly cleaned between 2 a.m. and the arrival of the prep-cook team four hours later. If he failed to do the work perfectly, the morning manager would scold him in front of the staff.
At home, he’d cry or fight with Afroz, who still hadn’t landed a residency placement. In addition to feeling degraded, Haider saw himself becoming estranged from his professional identity. “At work, people who were not as qualified as me would tell me I’m good for nothing,” he says. It was hard to not internalize that message.
Haider’s difficulties never reached the same extremes as those of his peers — a fact he partly attributes to his mutually supportive marriage — but his story offers a window into the tensions of his community. The high number of mental-health calls in Oakridge and Taylor-Massey indicates a neighbourhood in turmoil, but the more salient fact is that many such calls happen during crisis situations. According to data from the Toronto Central Local Health Integration Network, between 2012 and 2014, an average of 2,253 per 100,000 residents were hospitalized for mental-health conditions. No other East Toronto area comes close to matching that figure.
The data suggests a more extreme version of a familiar pattern. “We know that, when members of South Asian and East Asian communities present at psychiatric emergency departments, they’re much more unwell, compared to other ethnic groups,” says Virdee. Because of stigma and insufficient mental-health outreach, people do not always get the preventative counselling they need; when their pain becomes intolerable, they finally seek help, often at the ED . This tendency likely accounts for the dramatically high number of hospitalizations in Oakridge and nearby Taylor-Massey.
To address this crisis, Virdee argues, clinicians must get creative when it comes to outreach. “In larger mainstream services, the expectation is that people come to us,” she says. “But a culturally sensitive approach would mean providing services in places where people actually are.” For her, this means ensuring that religious leaders, who have immense influence in their communities, are equipped with counselling and referral skills. It also means expecting that non-medical personnel — settlement workers or employment counsellors — will provide pathways to psychiatric services. “In the health-equity field, we have a saying: ‘Every door should be the right door,’” says Virdee. “Wherever people show up for help, the staff should we well trained, the place should be welcoming, and the clients should be connected to the resources they need.”
“In larger mainstream services, the expectation is that people come to us. But a culturally sensitive approach would mean providing services in places where people actually are.”
The crisis in Oakridge won’t abate, however, unless Canada gets better at placing immigrants in suitable jobs. For Islam, such an improvement requires investments in skill-matching programs, bridge training courses, and mentorship initiatives. It also calls for tighter coordination between the federal immigration program and professional bodies. Otherwise, Canada, with its stringent application processes, is forcing immigrants to qualify for jobs they won’t get.
After their niece left in August 2016, Haider and Afroz started making new plans. “Please, find a way to be a doctor,” Afroz implored him. She was willing to uproot the family yet again, if that’s what it took. “You can start your career anywhere in the world,” she said. Haider got in touch with a friend from medical school, who was based in Saskatchewan but planned to practice in the UK. There, newcomers must pass two exams and an English proficiency test to get work. In the coming years, the disruption caused by Brexit will likely increase demand for foreign doctors, making UK residency placements easier to get than they are in Canada. Last November, after two tries, Haider passed the language test. Five months later, he visited the UK and successfully wrote his first exam. The couple hopes to relocate in early 2018. If Haider gains a specialty in family medicine, he may be able to return to Canada without a residency placement.
Despite the difficulties he faces, he still wants to settle in Toronto. He’d like to raise his children in a multicultural country — one that invests deeply in social services. His oldest son comes home from school and talks admiringly about Terry Fox and Viola Desmond; culturally, Canada feels like home. London, on the contrary, feels harsher and rowdier. “On the weekends, people drink, shout, and break bottles on the street,” he says. His experiences in Toronto, however, have made him wary of the so-called Canadian dream. “We’re hoping that someday we’ll be able to practice here. That’s the only thing keeping us alive,” he says. “If we knew before we came that it would be so hard, we probably wouldn’t have tried.”